Colorectal Cancer Surgery
What Is Colorectal Cancer Surgery?
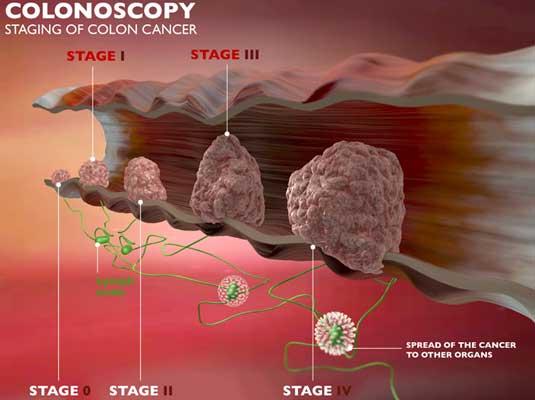
Colon and rectal cancers are cancer of the large intestine. These start out as polyps that slowly have a change in the DNA of the cells to the point that they become a cancer. Cancers are grouping of cells that grow abnormally and into areas where they aren’t normally seen. If left untreated, cancer will get larger and typically go to the liver or lung after first going to the lymph nodes in the area. These cancers can present with bleeding, blockage of the bowel (or narrowing of the stools), occasionally as a hole in the bowel, or on routine colonoscopy.
What Are The Symptoms Of Colorectal Cancer?
Colon and rectal cancer can present in a variety of ways. People can have bleeding (although the most common cause of blood in the stool is hemorrhoids) or bowel blockage. Sometimes people will feel a mass or just not feel that good.
How Is Colorectal Cancer Treated?
Colon and rectal cancer are addressed through a very orderly process. Once a patient is diagnosed with colon cancer, it is important to have an idea of the stage (with 1 being the best and 4 the worst) of the disease. This is where the two type of cancers diverge.
In colon cancer, scans are obtained to ensure that it hasn’t gone to the liver or lungs (stage 4 disease). If it hasn’t, most people should then get surgery to remove that portion of the colon along with the lymph nodes. Depending on the results from the surgery, some patients need no further treatment apart from close follow-up. Other patients need chemotherapy to treat any cells that may have traveled outside the area removed.
Rectal cancer can be more complicated. If the tumor has gone to a certain depth or if there are lymph nodes present, then patients will typically get chemotherapy and radiation prior to surgery. If the cancer is small enough, surgery may be the only treatment needed.
If the cancer has spread to other parts of the body like the liver or lungs, the patient may either end up getting surgery or chemotherapy depending on the details of the disease.
What Are The Complications Of Colorectal Cancer Surgery?
There are several variations to surgery that are used to treat colon and rectal cancer. The first determination is where the cancer is based (ascending, transverse, descending, sigmoid colon, or rectum), which will determine how much area needs to be removed. Depending on the size of the tumor, most patients are appropriate for a laparoscopic removal of the cancer (making small incisions and using a small camera and instruments). However, sometimes, depending on your surgeons judgment and expertise in laparoscopic surgery, an open approach may be a better option. The other consideration is whether a patient will need a colostomy (where a piece of bowel is brought to the abdominal wall and allows the patient to poop into a bag that sits on the abdominal wall for a period of time). Most patients do not need a colostomy and of the ones who do, most of the time it is reversible.
What Is My Recovery Time After Colorectal Cancer Surgery?
Most patients are in the hospital between one and seven days after surgery. You shouldn’t lift more than 10 pounds for 6 weeks. You shouldn’t shower for 2 days or take tube baths or swim for 2 weeks. You should get up and move as much as possible. People will often be sore for several days after surgery, but that gets better with time. Some people will have a poor appetite after surgery. There are no specific dietary restrictions after surgery. You can eat what you feel like.
Some surgeons use a protocol called Enhanced Recovery After Surgery (ERAS). Using this protocol, a patient is given a carbohydrate drink the day before and the day of surgery. Special injections are performed during the procedure and the patient is placed on a liquid diet right after surgery. It is very important to get up and move around as quickly as possible in order to help the bowel resume their normal function. The patient will take a couple of non-narcotic pain medications. The preference is for non-narcotic pain medications in order to decrease the need for narcotics and increase the speed of return of bowel function.
What To Ask A Breast Cancer Surgeon
Call Us
360.613.1335
Message Us
To request an appointment
Locate Us
Get directions to our office
